All Acne Is Not Created Equal. Your Guide To The Types And Treatments
At some point in your life, you've probably struggled with acne. If you're one of those people who left acne behind in high school, you're one of the lucky ones. Dr. Christopher Bunick of Yale Medicine says nearly half of women in their 20s, a third of women in their 30s, and a quarter of women in their 40s still struggle with acne. Men have it easier when it comes to acne, but about 12% of them also struggle with acne into their 40s.
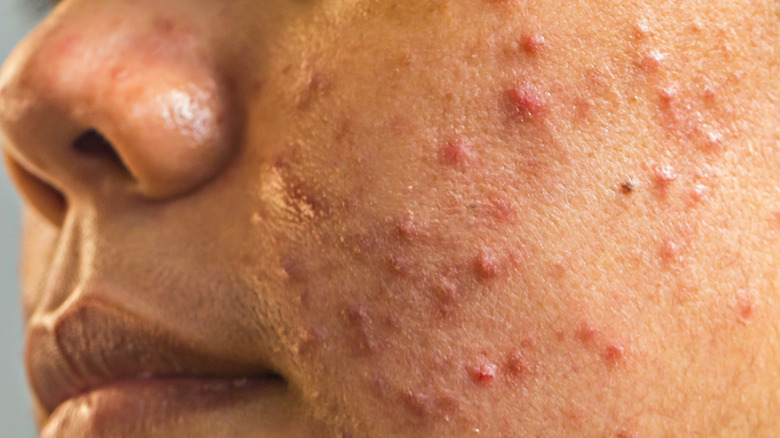
Acne is a broad term that covers a wide variety of skin blemishes. The ones you're probably most familiar with are whiteheads, blackheads, pustules, and papules. But there's also nodular acne, cystic acne, hormonal acne, and fungal acne. Who knew? It's a lot, but we'll walk you through all the different types, why they happen, and how to treat them.
Acne vulgaris
The most common form of acne, "acne vulgaris," encompasses all types of acne except for fungal acne. Contrary to popular belief, acne does not form when dirt clogs the pores in the skin. According to the Merck Manual, acne vulgaris develops when the skin produces too much of an oily substance called sebum. When the spaces around the hair follicles on the face, commonly referred to as pores, get clogged with this sebum, a blemish forms. When the pore is completely clogged, bacteria can build up in the pore, which triggers the body's inflammation process. Once the inflammation builds up, the blemish gets larger, eventually breaking the skin, resulting in what we know as pimples or zits.
Puberty is the most common trigger for acne because of the significant hormonal changes that occur during this developmental stage. Acne can also be triggered by the hormonal fluctuations that happen during the menstrual cycle. But hormones aren't the triggers of acne. Environmental factors like humidity and sweating can lead to excess sebum production, which can trigger acne. Makeup and beauty products can also block pores, leading to acne.
Non-inflammatory vs. inflammatory acne
Acne vulgaris is split into two categories: non-inflammatory and inflammatory. The experts at Acne.org point out that these categories are a bit misleading because technically all acne vulgaris triggers inflammation in the body. However, dermatologists still use these terms to differentiate between acne blemishes that are visibly inflamed and ones that aren't.
Whiteheads and blackheads are both considered non-inflammatory because the inflammation occurs on the inside of the pore and the blemish doesn't break through the skin. Though inflammation is happening, whiteheads and blackheads don't appear inflamed when you look at them in the mirror.
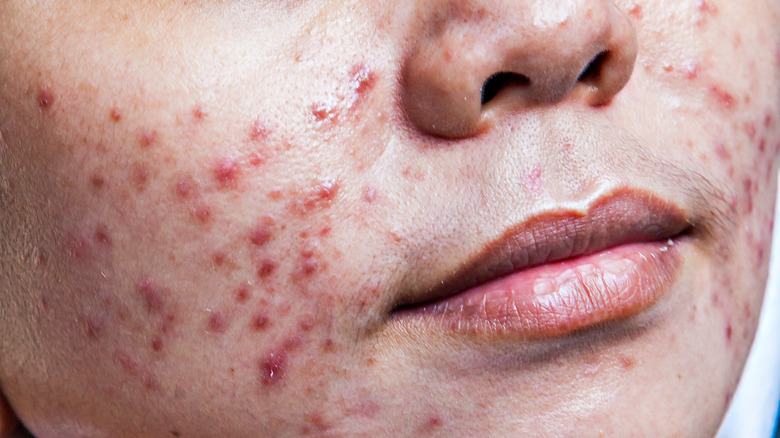
When bacteria starts to build up in an acne blemish and the inflammation increases, the blemish can break through the skin. This creates a red or white raised bump that's often painful to the touch. With this type of acne, the inflammation isn't just happening in the pore; it's also happening on the skin, where the blemish broke through. Inflammatory acne can come in many different forms, including papules, pustules, cysts, and nodules.
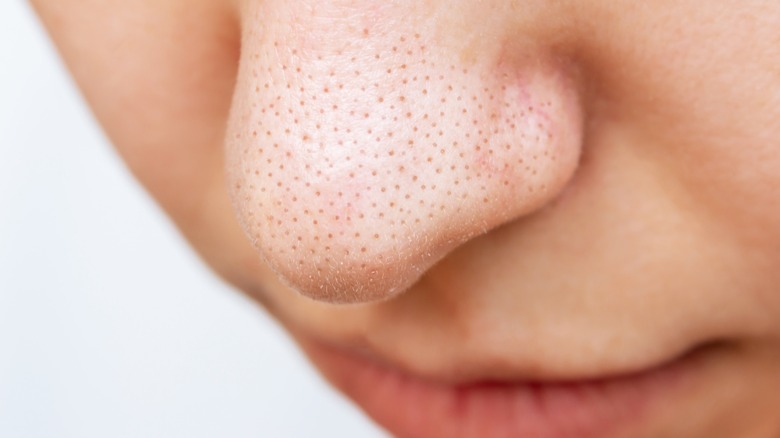
Comedones (aka whiteheads and blackheads)
We've mentioned both whiteheads and blackheads a few times already, but let's dig into what these little blemishes are and how they happen. The technical name for both whiteheads and blackheads is comedones (MedlinePlus). Comedones form when the space around a hair follicle, called a pore, is blocked. Sebum, skin cells, and bacteria build up in the pore; the pore gets inflamed; and a little black, white, or flesh-colored bump appears on the skin.
When the pore gets clogged close to the surface, it closes entirely. The sebum, skin cells, and bacteria all build up right under the skin, leading to a closed bump called a whitehead. When the pore gets clogged deeper down, the sebum, skin cells, and bacteria build up deep within the pore, leaving the top of the pore open on the skin. The opening of the pore gets exposed to oxygen, which reacts with the melanin — the substance that gives the skin its pigmentation — and turns the pore black. These blemishes are called blackheads.
Blackheads and whiteheads are the least severe form of acne. Sometimes, these blemishes will resolve on their own or with minimal treatment. But sometimes, blackheads and whiteheads get worse, turning into papules or pustules.
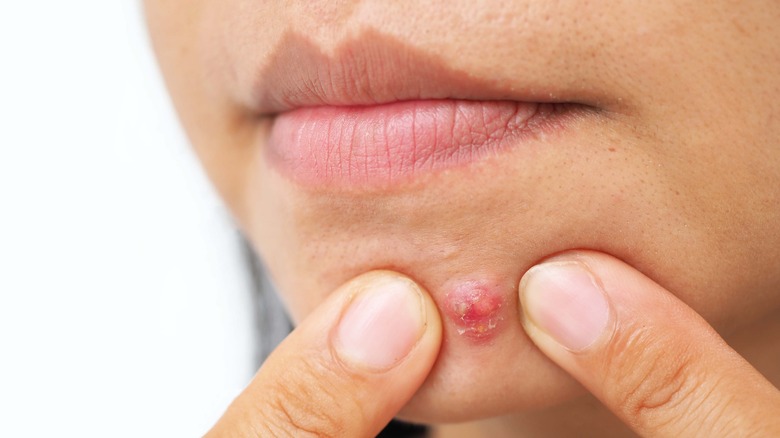
Papules and pustules
Papules and pustules all start out as either whiteheads or blackheads. Even if you didn't see a blackhead or whitehead before a pimple appeared, a tiny one was there, growing. When the blackhead or whitehead gets so full of sebum, skin cells, and bacteria that it bursts through the skin, it becomes a papule, per the Cleveland Clinic. Papules appear as rigid, inflamed bumps on the skin. They may look red, purple, or even brown due to the inflammation on the surface of the skin and inside the pore. Papules are typically hard and painful to the touch because they're so inflamed.
Most papules will go away on their own or with minimal treatment. However, if the infection in the pore worsens, papules can turn into pustules. When papules start to fill with whitish or yellowish pus, which is part of the immune system's response to an infection, they become pustules. These blemishes appear as lumps on the skin, usually larger than papules, with a whitish or yellowish tip because of the pus they contain.
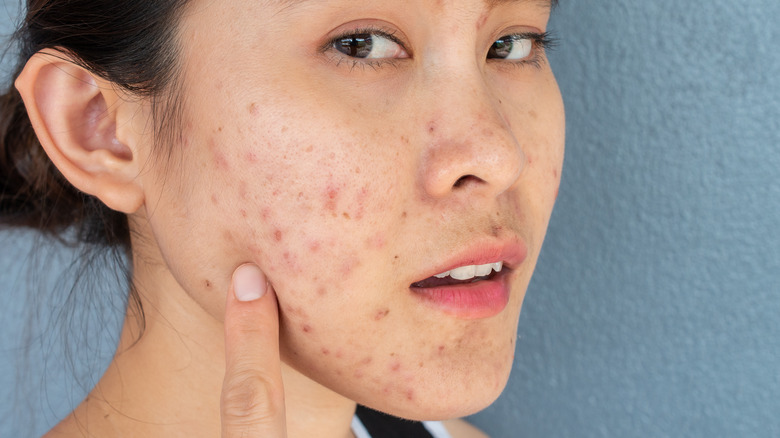
Cystic acne
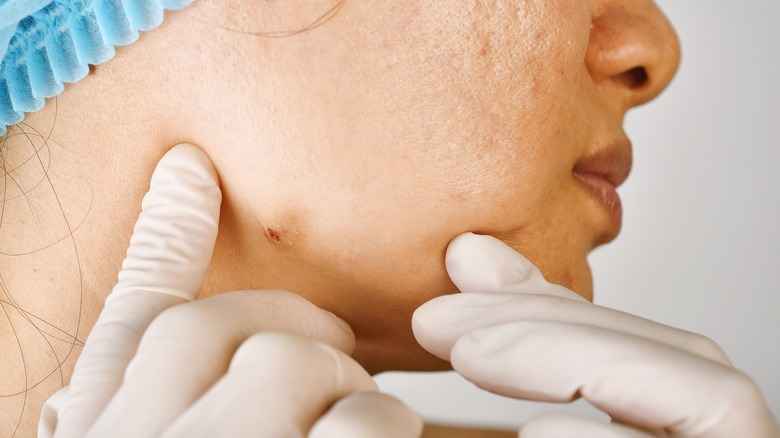
When an acne infection spreads to the deeper layers of your skin, pus builds up and forms a large bump on the skin called a cyst, according to WebMD. These cysts can be quite large, and they're often painful. Sometimes they're even itchy. Unlike less severe forms of acne, cystic acne can actually cause permanent damage to your skin. Even after the cysts are gone, they can leave tiny scars called icepick scars and larger cavities in the skin.
Cystic acne is one of the most severe types of acne, and it won't go away on its own. In fact, cystic acne can cause more breakouts by spreading the infection across the skin if the cysts break. It's important to consult a dermatologist if you think you have cystic acne because it probably won't resolve with over-the-counter acne medications, and if left untreated it will likely get worse.
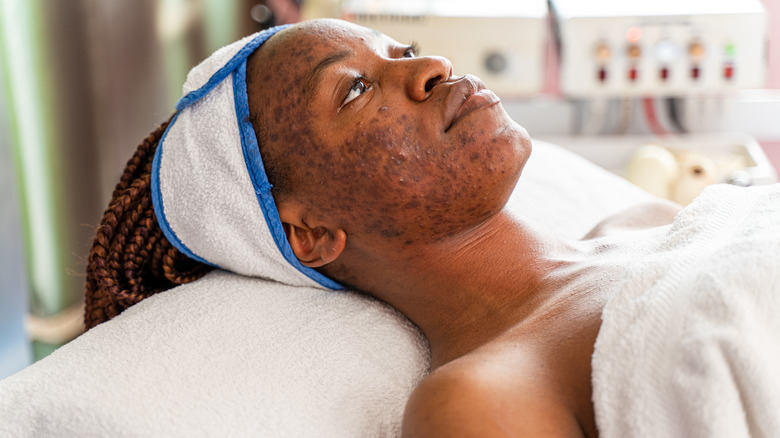
Nodular acne
Like cystic acne, nodular acne happens when a surface infection spreads deep below the skin, according to RxSaver. Unlike cystic acne, though, nodular acne blemishes don't fill with pus. Nodular acne shows up as solid bumps on the skin called nodules, hence the name.
Sometimes, the nodules are red and look inflamed, like cystic acne blemishes. In other cases, the nodules aren't discolored at all and just look like flesh-colored bumps on your skin. But even though nodular acne may not look inflamed the way cystic acne does, the nodules are still quite inflamed, which can make them painful to the touch.
Nodular acne is just as severe as cystic acne, and similarly, it won't just go away. Even with diligent treatment, it can take months or years for nodular acne to clear up. It's important to work with a dermatologist if you think you have nodular acne.
Hormonal acne
Although some may talk about hormonal acne as if it's an entirely different form of acne, it's really not. Hormonal acne is simply acne vulgaris — whiteheads, blackheads, papules, pustules, cystic acne, and/or nodular acne — caused by a hormonal imbalance. Dr. Erin Stigall, a dermatologist at the Dermatology & Skin Surgery Center of Wilmington, explains that hormonal acne is usually caused by an excess of hormones called androgens. These hormones exist in people assigned male at birth (AMAB) as well as people assigned female at birth (AFAB), though AMAB people naturally have much higher levels of androgens than AFAB people.
When androgen levels are too high in AFAB people, they can develop acne. This happens because androgens are tied to sebum production, and the body overproduces sebum when there's an excess of androgens. Though any acne can be caused by hormonal shifts or imbalances, medical professionals tend to use the term hormonal acne to describe persistent acne that doesn't resolve with typical treatment methods like over-the-counter acne products.
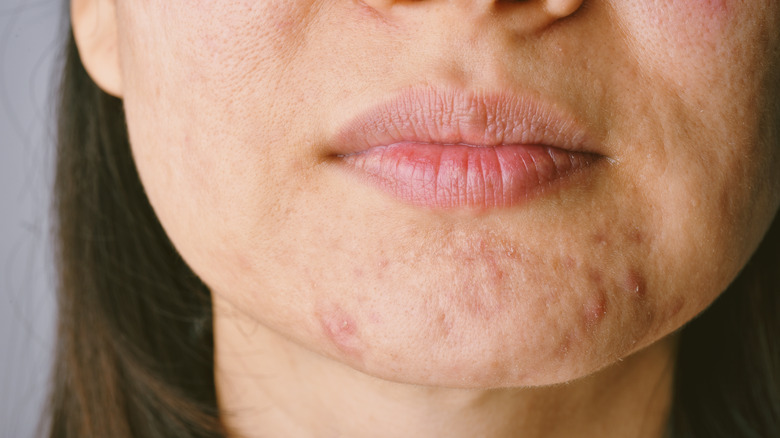
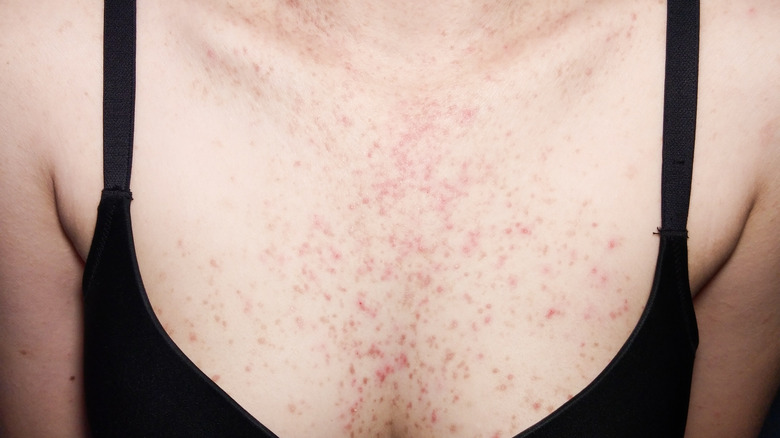
Like acne vulgaris, hormonal acne can show up anywhere on the face, neck, shoulders, or back. However, hormonal acne is most common around the jawline and chin. When people have persistent breakouts that mostly show up in those areas, hormonal acne is likely the cause.
Fungal acne
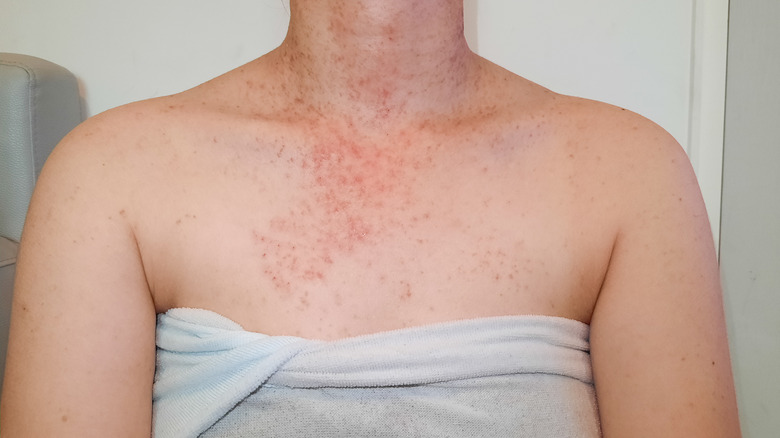
Pityrosporum folliculitis, commonly called fungal acne, is not actually a type of acne — specifically, because the condition isn't caused by sebum blocking the pores, according to Dr. Susan Massick of the Ohio State University Wexner Medical Center. Instead, so-called fungal acne is caused by an overgrowth of a specific kind of yeast that normally exists on the skin. Fungal acne often develops in the summer when sweat, humid weather, and heat combine to create the perfect environment for yeast to grow.
Fungal acne is often mistaken for acne because it causes red bumps that look a lot like inflammatory acne. The bumps are even located on hair follicles, just like acne blemishes. Unfortunately, if you treat fungal acne with antibacterial products, which are commonly used to treat acne vulgaris, you're actually creating an even better environment for the yeast that causes fungal acne. Antibacterial acne treatments essentially wipe out the skin's natural bacteria (which help prevent yeast overgrowth).
So, it's important to know when you're dealing with fungal acne, not acne vulgaris. The bumps caused by fungal acne often appear in uniform lines on the skin, not randomly like pimples or zits. Fungal acne is also itchy rather than painful like inflammatory acne.
Each type of acne needs a different treatment
If you've been trying to get rid of your acne for a while and it's just not clearing up, it's possible that you've been using the wrong products for the type of acne you're dealing with. According to the American Academy of Dermatology Association, there are three different approaches to treating mild to moderate acne, including whiteheads, blackheads, papules, and pustules. You can try treating the bacterial infection, reducing the amount of oil in the skin to unclog the pores, or treating the inflammation to unclog the pores. Mild to moderate acne will often respond to one of these treatments, but in some cases, you'll need to attack the breakouts on all three fronts.
If you're dealing with cystic acne, nodular acne, hormonal acne, or fungal acne, none of these approaches will work. Since cystic and nodular acne are more severe types of acne vulgaris, they often need prescription treatments. Hormonal acne needs a systemwide approach, and fungal acne requires a completely different treatment since it's not even really acne. So, it's really important to know which kind of acne you're dealing with before you try to treat it at home.
Acne treatment myths
Before we break down the best ways to treat each type of acne, let's bust some common myths about treating acne (hint: toothpaste on a zit isn't effective). A lot of people will tell you that you need to change your diet to get rid of acne. But according to the Merck Manual, your diet isn't what's causing your acne. There's some research that suggests certain foods can make existing acne worse, but the link isn't definitive. Some people do find their acne improves if they cut down on sugar, but you're not going to permanently clear up your breakouts by avoiding sweets.
In addition, though it seems counterintuitive, frequently cleansing or scrubbing acne prone-skin can actually make acne worse, because it reduces naturally occurring oils on the skin. Yes, an overproduction of oil is what causes acne, but you do need some oil on your skin, and when you get rid of it by overwashing, your body responds by producing even more oil, leading to more acne. You need to find the sweet spot that works for your skin.
Finally, if you've ever heard that tanning can reduce acne, don't try it! Tanning can slightly reduce the appearance of acne by changing your skin tone, but it doesn't do anything at all to treat acne. And it's really bad for your skin. So, just don't. Now that we've covered the myths, let's move on to what actually does work.
Treating whiteheads and blackheads
If you're just dealing with breakouts of whiteheads and blackheads, consider yourself lucky. According to WebMD, these types of acne are some of the easiest to treat because the blemish is close to the skin's surface and the bacterial buildup isn't too extensive.
You can usually clear up whiteheads and blackheads with over-the-counter treatments, which you can purchase at any grocery store or pharmacy. Look for products that contain benzoyl peroxide (which treats bacterial infection) or salicylic acid (which unclogs pores and reduces oil production). Keep in mind, though, cleansing with acne treatments more than twice a day won't make them more effective and will do more harm than good. If you get particularly sweaty, gently rinse your face with some water to make sure oil doesn't build up between washings.
When dealing with whiteheads and blackheads, it's important to make sure you don't irritate your skin as this can lead to more breakouts. So, when you're starting to treat your acne, use the gentlest product you can find for a few weeks. If you don't see improvements, try a slightly stronger product or find products with a different active ingredient. Always wash your face with lukewarm instead of hot water, and don't scrub too hard. If over-the-counter treatments don't work, talk to your doctor. You may need a prescription for a stronger cleanser or topical treatment.
Treating papules or pustules
Papules and pustules are harder to treat than whiteheads and blackheads. Dr. Sandra Lee, better known as Doctor Pimple Popper, explains that papules and pustules need more extensive treatment because there's more bacteria buildup and inflammation in the pores and on the skin.
The good news is that most breakouts of papules and pustules will still respond to over-the-counter treatments. Dr. Lee recommends using a combination of products containing benzoyl peroxide, salicylic acid, and retinol. Using all three of these active ingredients helps attack breakouts on all three fronts — fighting bacteria with benzoyl peroxide, fighting inflammation with retinol, and reducing oil with salicylic acid.
Your regimen will likely involve three steps — cleanse, treat, and moisturize — twice a day. Which active ingredients you use for each step depends entirely on your skin. You might use a salicylic acid cleanser, treatment cream or gel with benzoyl peroxide, and a moisturizer with retinol. Or maybe a benzoyl peroxide cleanser, treatment cream with salicylic acid and retinol, and a light moisturizer. You'll probably have to play around with your products and regimen to find what works. Be sure to give each product a few weeks before trying something new.
If your skin doesn't clear up with over-the-counter products, see a dermatologist. You might need prescription treatments or you may be dealing with cystic or nodular acne, which require totally different treatments.
Treating cystic acne
Because cystic acne is one of the most severe types of acne, it can be hard to treat, especially on your own. Dr. Mona Gohara from Dermatology Physicians of Connecticut told NBC News that most cystic acne won't be cleared up by over-the-counter treatments. "Topically, it's really hard to treat cystic acne — over-the-counter products may help mitigate the inflammation and bring it down a bit, but making it go away is a lot trickier and they will not be effective if used alone," she said.
Cystic acne really needs to be assessed by a dermatologist, Gohara continued. They can develop a treatment plan based on the severity of your cystic acne and your skin. Usually, cystic acne will require systemwide treatment with oral prescription medications like antibiotics, retinoids, or birth control. Sometimes, a dermatologist may recommend cortisone injections to treat the cysts.
Though over-the-counter treatments won't get rid of cystic acne, a skincare regime with over-the-counter products is still an important part of managing the condition. Dr. Tracy Evans, a dermatologist from Pacific Skin and Cosmetic Dermatology, told NBC that people with cystic acne should be "cleansing your skin with a wash that contains salicylic acid or alpha hydroxy acid at least a couple of times a week and moisturizing with an oil-free moisturizer that's gentle on the skin."
Treating nodular acne
Like cystic acne, nodular acne won't clear up entirely with over-the-counter treatments. You'll need to see a dermatologist who can assess your nodular acne and come up with a treatment plan.
According to a paper published in the American Journal of Clinical Dermatology, one of the most effective treatments for nodular acne is a prescription medication called isotretinoin, a retinoid that comes in pill form. People who don't respond well to retinoids may be prescribed oral antibiotics instead. In some cases, your dermatologist may suggest cortisone shots to treat the inflammation associated with nodular acne. Some people also respond well to hormonal birth control.
In addition to prescription medications or cortisone injections, you'll need a thorough skincare regimen to manage nodular acne. Products that contain benzoyl peroxide and retinoids are the most effective at treating nodular acne. Talk to your dermatologist about which products work best with your treatment plan and how often to use them.
Treating hormonal acne
When your acne is caused by hormonal shifts or a hormonal imbalance, none of the typical treatments will completely clear up your skin. You may see some improvement from over-the-counter products or prescription-strength topical treatments, but your acne won't go away until you treat the underlying hormonal issues.
A paper published in the International Journal of Women's Dermatology states that treating hormonal acne with birth control pills can significantly reduce, or even eliminate, breakouts. Birth control reduces androgen levels, and acne is often caused by excess androgen in the body. Another prescription medication called spironolactone, which blocks some androgen production, is also effective for hormonal acne. Often, dermatologists will prescribe both birth control pills and spironolactone for extra effectiveness. Since both these medications require a prescription, you'll need to see a dermatologist to start hormonal medications for acne.
Like other forms of acne that are treated with oral medications, an at-home skincare regimen is still an important part of managing hormonal acne. According to the Cleveland Clinic, your skincare routine for hormonal acne depends on what kind of blemishes you have. For blackheads and whiteheads, a prescription topical cream called tretinoin may help. Over-the-counter or prescription products containing benzoyl peroxide or retinoids may help with papules or pustules. If your hormonal acne triggers nodular or cystic acne, follow a treatment plan developed by a dermatologist.
Treating fungal acne
Because fungal acne isn't actually acne, you'll never get completely clear skin with acne treatment. Dr. Michele Green, a dermatologist based in New York City, explains that because fungal acne looks so much like acne vulgaris, it's nearly impossible for us regular folks to identify what we're dealing with. When your acne isn't clearing up, or is getting worse with over-the-counter treatments, it's time to head to the dermatologist so you can get a professional diagnosis.
If your dermatologist says you're dealing with fungal acne, they'll come up with a treatment plan based on the severity of your case. The basis of that treatment plan will be antifungal medications rather than antibacterial medications. The dermatologist may prescribe topical antifungal creams like Nizoral or Clotrimazole or oral antifungal medications like Fluconazole. They may also recommend that you wash your body with an antifungal shampoo like Selsun Blue.
Over-the-counter antifungal creams may also help with fungal acne, but you need to know that you're dealing with fungal acne rather than acne vulgaris before you try them. If you've dealt with fungal acne in the past and you think you're having another breakout, you can try washing with antifungal shampoo and applying over the counter antifungals before heading to the dermatologist for prescription treatments.